|
The primary aim for this systematic review and meta-analysis was to assess whether pharmacological interventions when compared to placebo, or other pharmacological/psychosocial interventions resulted in a clinically significant reduction or prevention of symptoms, improved functioning or quality of life, presence of disorder, or adverse effects. Its occurrence after a severe traumatic event and association with characteristic neurobiological changes make PTSD a good candidate for pharmacological prevention and early treatment. This definition encompasses the depersonalization and derealization symptoms identified in the PTSD dissociative subtype (feeling detached from the self or environment).ĭissociation can also include memory impairment, particularly loss of memory of traumatic events reduced response to the environment (physical and emotional numbness) spontaneous “trancing” or “spacing out” and identity confusion or fragmentation ( Lanius et al., 2016).Post-traumatic stress disorder (PTSD) is a common mental disorder associated with significant distress and reduced functioning. However, 15 to 30 percent of people with PTSD, particularly those with chronic childhood traumatization, have over-modulated traumatic emotions and responses, manifested as dissociative symptoms ( Lanius et al., 2016).ĭissociation is “a disruption of the usually integrated functions of consciousness, memory, identity, or awareness of body, self, or environment” (APA, 2013). Many of the symptoms captured in the core diagnostic criteria for PTSD represent hyperarousal symptoms, or under-modulation of the central nervous system in response to trauma-related cues. People with a history of complex trauma are more likely to develop symptoms after subsequent adulthood trauma ( Herman, 1997 Lanius et al., 2016). People with such complex traumatization are more likely to present with dissociative symptoms, somatization, extensive comorbidity, intense suicidality, and alterations in identity and interpersonal relatedness. Because the latter occurs repeatedly during critical developmental periods, it interrupts or prevents normal developmental tasks such as consolidating identity, forming basic trust in others and learning affect regulation skills (Glaser, 2000 Herman, 1997). The impact of a single event in adulthood is different from the impact of repeated childhood sexual or physical victimization or neglect by a primary caregiver. The heterogeneity in the clinical presentation of PTSD can be partly explained by significant differences in the types, patterns and timing of traumatic events. A study of primary care patients who met criteria for PTSD found poorer overall health functioning and higher rates of using health care services ( Gillock et al., 2005). 
PTSD may also present as somatic symptoms and frequent use of the medical system. The person may experience prominent feelings of guilt and shame, and a sense of “moral injury.” In military populations, guilt and shame are associated with later development of PTSD ( Nazarov et al., 2015). Other common presentations include low mood, anxiety and panic, specific phobias, anger problems, insomnia or nightmares, interpersonal difficulties, occupational dysfunction and emotional numbness. PTSD may also present as profound dysphoria and anhedonia, significant irritability and behavioural reactivity, or persistent dissociation and detachment. It has been moved into a new category called “trauma and stressor-related disorders.” This separate classification acknowledges that not all people with PTSD have a presenting complaint related to anxiety. In DSM-5, PTSD is no longer classified as an anxiety disorder. (See Diagnosis for full DSM-5 diagnostic criteria.) 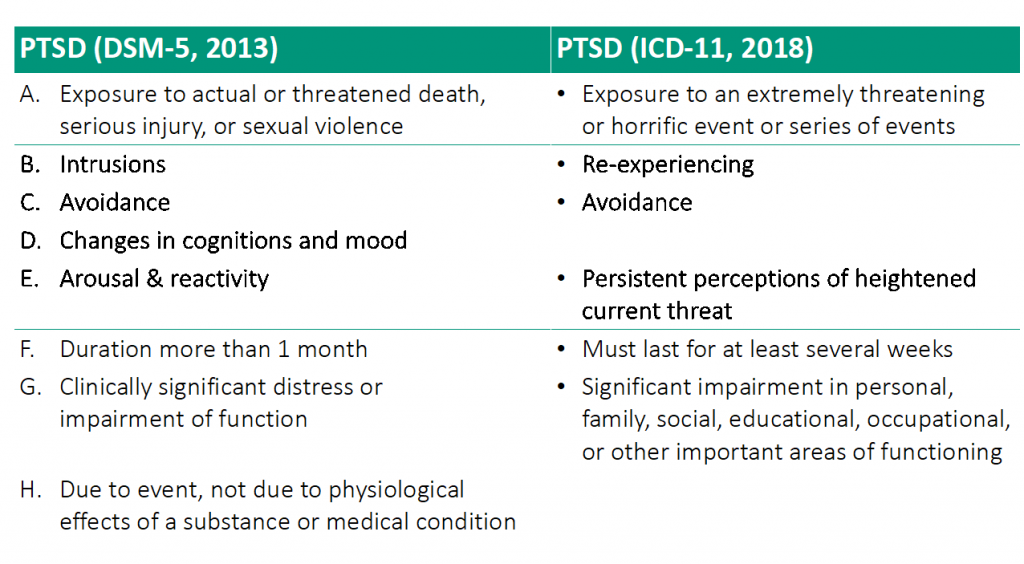
Symptoms must be present for more than one month and result in significant distress or impairment. The person must experience symptoms across four clusters: intrusions, avoidance, negative alterations in mood or cognition, and alterations in arousal. The first diagnostic criterion for PTSD is having experienced a traumatic event, which DSM-5 defines as “exposure to actual or threatened death, serious injury, or sexual violence” (APA, 2013). The DES cannot be used for diagnosis, but scoring over 20 per cent indicates the need to further explore dissociative symptoms ( Lanius et al., 2016). The general population average is 4 to 8 percent compared with 26 to 42 percent among people with PTSD ( Carlson & Putnam, 1993). 
The self-report Dissociative Experiences Scale (DES) asks respondents to rate what percentage of the time they experience a given dissociative symptom ( Bernstein & Putnam, 1986).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
